What Is TMJ Disorder? Symptoms, Diagnosis, and Treatment
Jaw pain that makes eating uncomfortable, a clicking sound when you open your mouth, or headaches radiating from just in front of your ears are among the most common signs of a temporomandibular disorder. These symptoms are more widespread than many people realize. Studies estimate that TMD affects up to 12 million adults, with most cases occurring between the ages of 20 and 40. Women are approximately twice as likely to develop the condition as men.
Despite how common it is, TMD is frequently misdiagnosed or left untreated for extended periods. Understanding what the condition involves, what causes it, and how it is managed helps you make informed decisions about your care.
What Is the Difference Between TMJ and TMD?
The temporomandibular joint is a sliding hinge joint located just in front of each ear. It connects the lower jaw to the skull and enables the movements involved in chewing, speaking, and yawning. There is one joint on each side of the face.
TMD, or temporomandibular disorder, refers to the group of conditions that affect this joint and the muscles controlling jaw movement. While many people use "TMJ" as shorthand for the disorder, the accurate clinical term is TMD. The distinction is relevant because TMD encompasses several different problem types, each with its own cause and treatment pathway.

What Causes TMJ Disorder?
The exact cause of TMD is often difficult to determine. In many cases it develops from a combination of factors rather than a single identifiable source.
The most commonly identified contributing factors include teeth grinding or clenching (bruxism), jaw injuries such as fractures or dislocations, arthritis affecting the joint cartilage, bite misalignment where the upper and lower teeth do not meet correctly, and chronic stress that leads to persistent jaw tension.
Certain habits can worsen existing symptoms without causing TMD directly, including:
Chewing gum excessively or biting hard objects such as ice or pens
Taking large bites of food or using teeth as tools
Clenching during the day or sleeping on your stomach
Poor posture, particularly forward head positioning, which places additional strain on the jaw muscles over time
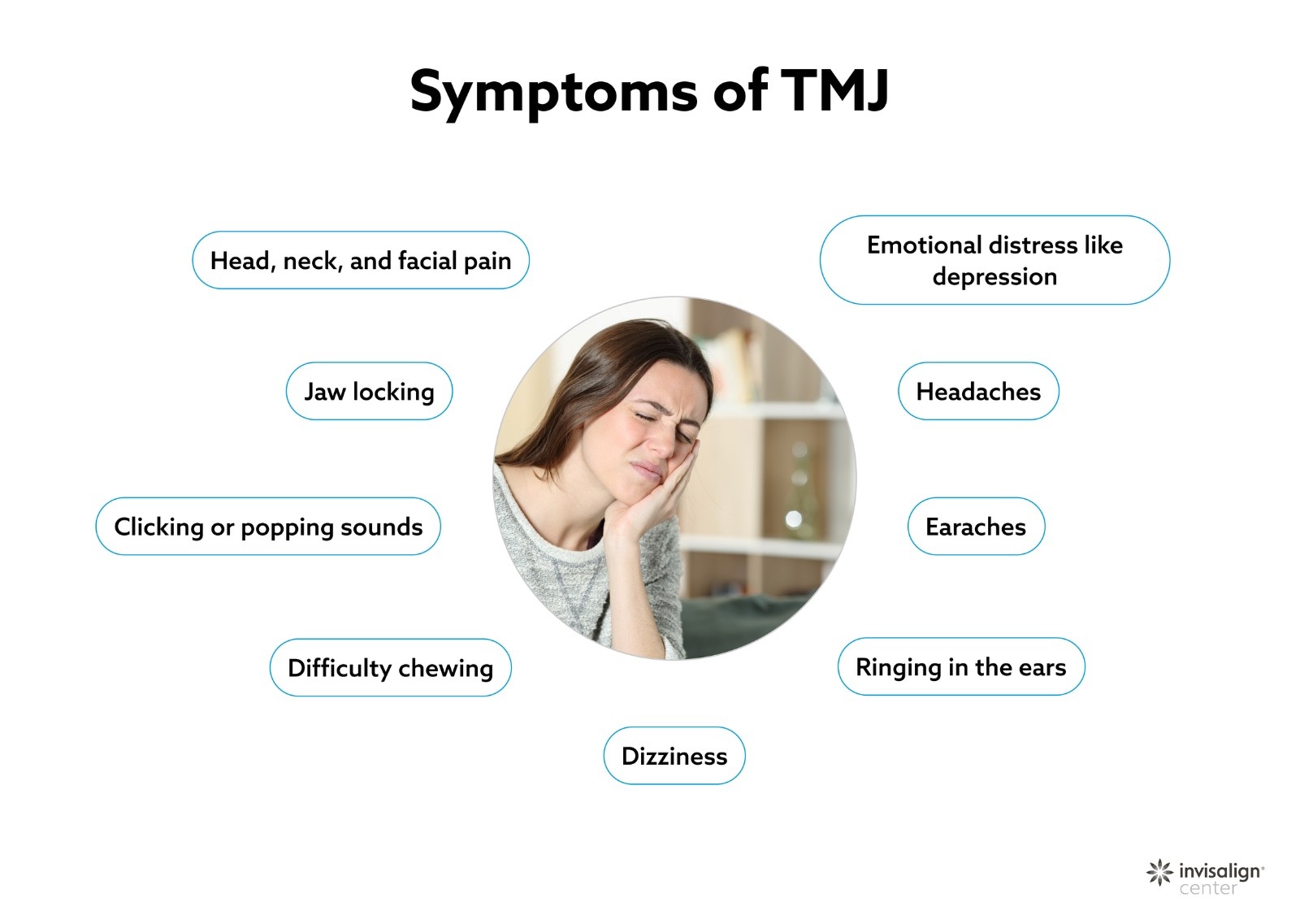
What Are the Symptoms of TMJ Disorder?
People experience this condition very differently. The most frequently reported symptoms include pain or tenderness in the jaw or face, aching pain in or around the ear, difficulty or discomfort while chewing, clicking or popping sounds when opening or closing the mouth, jaw stiffness, and locking of the joint. Some patients also experience headaches, neck or shoulder pain, eye pain, and tooth pain alongside jaw tenderness.
It is worth noting that clicking or popping sounds alone, without accompanying pain or restricted movement, do not necessarily indicate a disorder requiring treatment.
TMD symptoms closely resemble those of several other conditions, including cervical spine disorders, sinus problems, ear conditions, and certain types of headache. This overlap makes accurate diagnosis important before any treatment is started.
How Is TMJ Disorder Diagnosed?
A specialist will begin with a physical examination, assessing how widely you can open your mouth, pressing around the jaw to identify areas of tenderness, and feeling the joints as you open and close your mouth. They will also evaluate your bite for any misalignment contributing to joint strain.
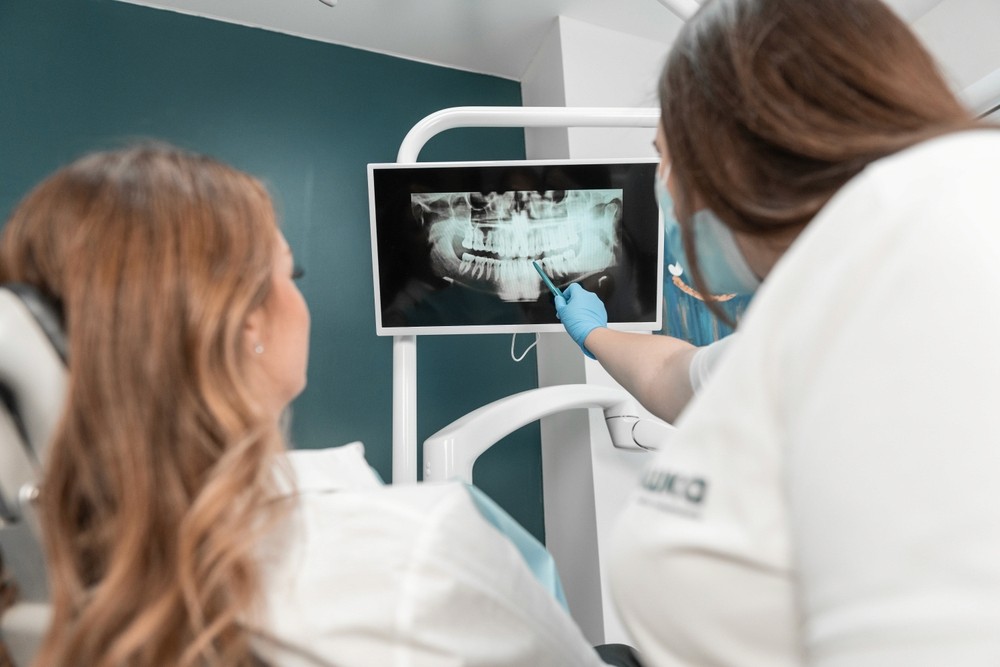
If the physical examination does not provide a complete picture, imaging tests offer a more detailed view. These may include dental X-rays to assess bony structures, CT scans for a three-dimensional view of the bones, or MRI when soft tissue evaluation is needed, particularly to assess the disc position inside the joint. In cases where jaw structure and skeletal relationships are a factor, an orthognathic assessment may also be appropriate.
To support an accurate assessment, it helps to come prepared. Sharing a complete medical history with your specialist, including recent injuries, known health conditions, and a note of when symptoms tend to be worst, reduces the risk of misdiagnosis and ensures the evaluation is as thorough as possible.
What Are the Treatment Options for TMJ Disorder?
Most people with TMD improve with non-invasive approaches. Surgery is considered a last resort and is only recommended when conservative measures have not produced sufficient improvement.
Oral Appliances
A custom-fitted splint or night guard worn during sleep reduces joint load by limiting clenching and repositioning the jaw in a more neutral alignment. Custom-fitted devices are generally more effective than over-the-counter alternatives because they are shaped precisely to your bite.
Physical Therapy
Targeted jaw exercises help restore range of motion, reduce muscle tension, and address posture in the neck and shoulders, which directly influences jaw position. This is one of the most effective non-invasive approaches available through physical therapy.
Medications
These typically include NSAIDs such as ibuprofen or naproxen, muscle relaxants for patients whose primary symptoms are clenching-related, and in some cases low-dose antidepressants used specifically for their effect on chronic pain modulation.
Other Non-Surgical Options
Additional approaches include trigger point injections using dry needling or corticosteroids to relax painful muscle areas, ultrasound therapy to improve blood flow and reduce muscle tension, and TENS therapy using gentle electrical currents to ease jaw tension.
Behavioral Changes
Avoiding hard or chewy foods, reducing habitual clenching, improving posture, and managing stress through consistent relaxation practices all reduce the daily load placed on the joint. Where bite misalignment is identified as a contributing factor, orthodontic treatment may be recommended as part of a broader care plan.
Surgical Options
When conservative treatment has not produced sufficient improvement, options range from arthrocentesis, the least invasive procedure, to TMJ arthroscopy through a small incision, to open-joint surgery for the most complex structural cases.
Can TMJ Disorder Be Prevented?
Prevention is not always possible, particularly when the cause is structural or genetic. However, several consistent habits reduce the cumulative strain on the joint over time:
Wear a night guard if you grind or clench your teeth
Use appropriate protection during contact sport
Maintain good posture, particularly in the neck and shoulders
Manage stress through regular physical activity or relaxation practices
Why Early Assessment Matters
Symptoms that are identified and addressed early respond considerably better to conservative management than cases where the condition has been present for years without intervention. With early diagnosis and the right treatment approach, TMD is often manageable and in some cases fully resolved.
When Should You See a Specialist
If jaw pain, clicking, or stiffness persists for more than two to three weeks, or if symptoms are affecting your ability to eat, speak, or sleep comfortably, a professional assessment is the appropriate next step. Many cases of TMD respond well to early conservative care, and the sooner the underlying cause is identified, the more straightforward the treatment path tends to be.
Frequently Asked Questions
Can I live a normal life with TMJ disorder?
For most people, yes. The majority of TMD cases are manageable with conservative treatment, and many resolve on their own over time. Some patients require ongoing management, particularly if the underlying cause involves a structural or chronic condition. With the right care plan, most people return to normal daily activities without lasting limitations.
What foods should I avoid with this condition?
Hard, crunchy, or chewy foods place the most strain on the joint. These include raw carrots, hard bread, tough meats, chewing gum, and ice. During flare-ups, softer foods such as cooked vegetables, fish, eggs, and yogurt reduce the load on the jaw and allow the surrounding muscles to rest.
Does sleep position affect TMJ disorder?
It can. Sleeping on your stomach or on the side of the affected jaw places direct pressure on the joint overnight and can worsen morning stiffness and pain. Sleeping on your back with a supportive pillow that maintains neutral head and neck alignment is generally the most comfortable position for people managing this condition.
Can a vitamin deficiency cause jaw joint problems?
There is no direct evidence that a specific vitamin deficiency causes TMD. However, deficiencies in magnesium and vitamin D have been associated with increased muscle tension and joint discomfort, which may aggravate existing symptoms. If you suspect a nutritional deficiency, a medical evaluation is the appropriate first step.
Is TMJ disorder serious?
For most people, it is not a serious condition in the long-term sense. It can, however, significantly affect quality of life when left untreated, leading to chronic pain, disrupted sleep, and difficulty eating. Cases that go unmanaged for extended periods are also more likely to require more involved treatment. Early assessment and appropriate care typically prevent the condition from becoming a long-term problem.


